Often inspiration strikes when you least expect it, and that was certainly the case with the personal ventilation hood.
In March 2020, intensive care specialist Dr Forbes McGain was thinking of his peers on the frontline of COVID-19 care, while jogging and pushing his daughter in a pram.
Inspired by the pram’s retractable hood, Dr McGain, from Western Health, contacted the head of Mechanical Engineering at the University of Melbourne, Professor Jason Monty, and the pair began discussing an idea to help reduce the spread of COVID-19 in hospitals.

Professor Monty assembled a team of mechanical engineering specialists who worked through the night to develop a prototype ventilation hood within 48 hours of their first conversation.
“Our University of Melbourne team really had to pivot and work outside their area of expertise,” says Professor Monty. “Things like patient comfort and interaction of people with devices is not something we usually deal with [in mechanical engineering].”
A fully mobile device, the personal ventilation hood (now licensed as the McMonty by medihood) is a transparent, plastic cover fitted over a hospital bed and the upper body of a patient. A small fan and special filter extract aerosol droplets, significantly reducing the infection risk of COVID-19 from patient to healthcare worker.
Thanks to the generosity of donors who contributed to the University’s COVID-19 Research Response Fund, the project received a grant of $55,000. This financial support resulted in 20 locally made hoods.
In November 2020, the McMonty by medihood was approved and deployed in clinical trials across Victoria, where it was used in treatment of more than 100 patients in intensive care units (ICU) alone.
The hood has since provided a sense of comfort to frontline staff, who, according to Professor Monty, have been grateful for the extra layer of protection while treating potentially infectious patients in intensive care.
“I was very conscious of how these hoods could save lives. We could see the concern among the [hospital] workers and feel the tension. After the first demonstration of the prototype at Footscray Hospital, there was extreme gratitude.”
Small cost, Big impact
Samantha Bates, Western Health’s Lead Research Manager, has spent more than 13 years working on clinical studies and said the hood’s impact has been ‘game-changing’.
“I can’t begin to describe how much anxiety and tension there was in intensive care when COVID-19 hit. People were worried about contracting the virus, yet when the device arrived and staff were educated on how to utilise it, we saw a change in people’s behaviour; everyone became more comfortable.”
In open-plan ICUs like the one at Footscray Hospital, curbing the spread of COVID-19 amongst healthcare workers was one of the biggest challenges faced by experts.
However, according to Dr McGain, healthcare workers were universally accepting of the device.
“During the initial clinical trial, we asked staff whether or not they felt less likely to develop COVID-19 because of the hood. 100 per cent of those who responded said that they felt safer with the hood,” says Dr McGain.
Of all Victorian hospitals, those managed by Western Health saw some of the highest numbers of suspected and confirmed COVID-19 patient admissions, resulting in significant numbers of healthcare workers, specifically nurses, being infected. Yet despite this, ICU nurses at Western Health recorded very low infection numbers when compared against other hospital wards.
Dr McGain says there could be many reasons for this, noting the hood played a pivotal role in helping to keep staff safe during the peak of COVID-19 at Western Health.
“A nurse who had been on maternity leave said to me ‘I came back during COVID because I knew the hood was going to protect me.’ And that was gold, because I hadn’t really thought of that.”
“I do think that our ICU is safer because of the hood. And it’s not just my opinion. If you ask the nursing staff that view is unanimous,” says Dr McGain.
Although the role of the initial design was primarily to protect healthcare workers from infection, patients also felt safer, and Samantha Bates says an unexpected win was how well it was received by patients in intensive care.
“We had an immunocompromised patient suspected of having COVID-19 who normally comes in and stays by himself in an isolation room. His feedback was that he quite enjoyed [being under the device] because he wasn’t alone in a room, he felt more cared for, he could talk to staff and feel part of the ward.
“Other patients described that the hood was like being comforted: like in a little bubble, which was lovely. It was overall really well tolerated by patients.”

Life after COVID-19
The hood’s impact doesn’t end at Western Health. The clinical trial has been extended across Australia, with Royal Hobart and Alice Springs being joined by Royal Melbourne, St Vincent’s, the Northern and Austin Hospitals, who have all agreed to continue testing the device.
As COVID-19 numbers nationally trend downwards, hospital departments are looking to the hood and how it can be put to use in the future.
As more and more hospitals gained knowledge of this new device and its success, it became clear to Samantha Bates that it could have a far larger impact beyond the intensive care ward.
“We’ve had interest from a number of different clinical areas. I’m talking to areas like the coronary care unit, the dialysis unit and the respiratory ward. With just one look at it, they would start telling me how they could use it within their own areas,” she says.
We actually had one of our anaesthetists, who collaborates with sleep scientists and respiratory people to do cardiopulmonary testing, reach out and ask if we could fit a hood to an exercise bike.”
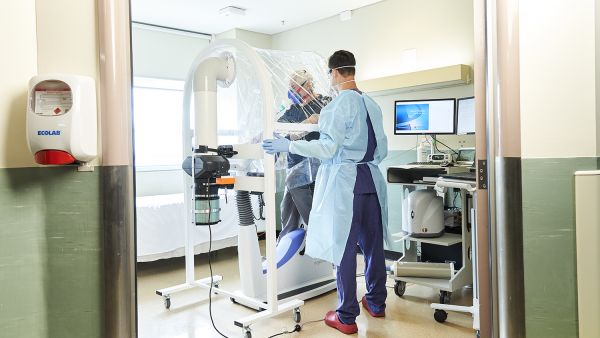
Exercise bikes are used in cardiopulmonary testing by anaesthetists to assess whether patients are physically able to undergo major surgery. However, because of COVID-19, these tests were stopped by hospitals due to the amount of aerosol particles patients generated while exercising.
Now with a hood fitted firmly over the bike, specialists can once again safely work in close proximity to their patients.
“Up until that point the program had been shut down for many months because of COVID, so there were many patients that needed to have this assessment done and could because the hood helped keep health workers safe while testing the patient,” says Samantha.
And according to Professor Monty, the hood was always envisaged by him and the engineering team as a device that could be used beyond the ICU.
“It’s incredible to think how far reaching the benefits of the hood are – that the solution we found to protect staff in the ICU can be applied to many more clinical settings.”
Another one of the unintended positives from the hood’s creation has been its impact on Victoria’s economic recovery.
Without the support from University of Melbourne donors and Western Health, this would never have got off the ground.
Made possible through the generosity of our donors, the initial funding grant was enough to secure 20 prototypes. However, because of its success, additional funding has been secured to locally manufacture more devices.
“We make these in West Heidelberg, it’s locally made and we’re using intellectual product and effort all homegrown in Melbourne,” says Dr McGain.
“And, without the support from the University of Melbourne donor community and Western Health, this would never have got off the ground.”